Open Shoulder Surgery
DIET
- Start with clear liquids (jello, soup broth, Gatorade, etc.), crackers, white bread and other light foods
- Progress slowly to heavier foods as you tolerate the lighter foods without any nausea
WOUND CARE
- Keep your dressing clean and dry and in place for seven days after surgery unless instructed differently by Dr. Roth.
- If Dr. Roth tells you that you have a waterproof dressing, you may shower with your dressing on. Otherwise, do not shower until instructed to do so by Dr. Roth.
- Once the incisions are completely dry for 24 hours, you may shower. Let the water and soap run over the incision and pat it dry with a clean towel after the shower. Do not scrub the incision or vigorously dry it.
HYGIENE
- You may prefer to keep a gauze pad or towel in your armpit while the arm is in the sling to keep the skin from chaffing
- When you are permitted to shower, you will not be able to lift the arm up over your head to wash under your armpit. A nice trick is to bend forward at the waist, and just let the arm dangle. This will allow gravity to open up the space under your armpit so that you can wash under your armpit without using any of the muscles of your shoulder. (This is essentially the same position you will be in when you do your pendulum exercises, described below in the EXERCISE section.)
CLOTHING
- Generally, putting on a shirt or sweatshirt with buttons or a zipper on the front (e.g. button-down shirt, hoodie, etc.) is easiest to wear after shoulder surgery, as compared to a shirt that has to be pulled over your head (e.g. t-shirt, pullover sweater, etc.).
- When putting on a button-down shirt, let the operative arm dangle, and use the good arm to pull the shirt sleeve over your operative arm FIRST, then reach back with the good arm to find the other arm hole and put the other sleeve on.
- When taking off a button-down shirt, reverse the process described above for putting it on – first take off the sleeve with the good arm, and then use the good arm to help take off the sleeve on the operative arm.
- In the beginning, sweat pants or looser fitting pants that can be pulled up with one arm are usually easiest to put on
- Slip on shoes are usually easier in the beginning than shoes with laces that need to be tied
- Similarly, socks can be difficult in the beginning with just one hand, and you may need someone to help you put socks on, or choose to wear shoes without socks until you are able to put them on on your own
MEDICATIONS
In many situations, your surgery will be performed at an ambulatory surgery center and you will be able to be discharged immediately after surgery to go home. Depending on your injury and the surgery performed, in some situations, you may need to spend a day or more overnight in a hospital. If you are staying in the hospital, Dr. Roth and the nurses will be managing your pain medications directly, and the following section will not be applicable yet. The following section should be referred to if you are going home directly after surgery.
- It is important to know that there will be some pain after surgery – this is very normal. Unfortunately, there is no such thing as “painless surgery.” While pain can sometimes be a marker of something going wrong, in the context of surgery, it is usually completely normal. If you are concerned about the level of pain that you are experiencing, please call Dr. Roth’s office and he and his team can discuss with you and ask a few questions to confirm that your level of pain is normal and not a sign of something dangerous.
- Dr. Roth uses the pain scale from 0-10 to try to help recommend how many opiate pain pills to take, so try to be honest with yourself about your pain level. Remember, zero is no pain at all, and 10 is the worst pain in the world. Dr. Roth recommends not taking any opiates if your pain is in a 0-4 range. Pain in the range of 0-4 is generally expected and very normal. If your pain rises above a 0-4, use the charts below for some recommendations of how to add in opiate medication to try to bring it down to the 0-4 range.
- You have been given a prescription for an opiate pain medication (Oxycodone, Percocet, Norco, etc.). By following the “Over-The-Counter Medicine” Regimens below, you may be able to avoid taking any of the opiate medication, or may only need it for a day or two. Feel free to wean off the opiate as soon as you can.
- If you have a history of Obstructive Sleep Apnea (OSA), be sure to let Dr. Roth know as he may decide to change your post-operative pain regimen.
- If your narcotic pain medication has ACETAMINOPHEN in it (e.g. Norco, Percocet) then you CANNOT also take TYLENOL at the same time, which is the same medication .
- Side effects of the pain medication include itching, nausea, vomiting, dry mouth, constipation, dizziness and lightheadedness. Taking the medication with food will decrease the risk of nausea. To prevent constipation, it is recommended that you take a stool softener (e.g. Colace) while taking the opiate. Colace can be purchased over the counter. Take one tab 2-3 times per day.
- If taking the opiate medication causes you to experience itching without a rash, and without any swelling of the mouth or difficulty breathing, this is very common, and is not a true allergy. The best way to manage this is to try to wean off the opiates and just take the Advil/Tylenol regimen described below, or to take Benadryl for the itching. However, the Benadryl may not manage the itching very well, and often just puts you to sleep so you aren’t as bothered by the itching.
- Try to wean off of the opiate pain medication as soon as possible. Using Dr. Roth’s regimen below will help you transition away from the opiates as soon as possible
- Dr. Roth’s Suggested Post-Operative Pain Management Regimens
(Note that generic medications are exactly the same as brand name and can be substituted at lower cost and without any change in effectiveness.)
|
DR. ROTH’S SUGGESTED OVER-THE-COUNTER PAIN REGIMEN MODERATE PAIN DO NOT take the Tylenol if your opiate has acetaminophen in it already (e.g. Percocet, Norco)
|
|
|
6 AM |
600 mg Advil (ibuprofen) 1000 mg Tylenol (acetaminophen) |
|
12 NOON |
600 mg Advil (ibuprofen) 1000 mg Tylenol (acetaminophen) |
|
6 PM |
600 mg Advil (ibuprofen) 1000 mg Tylenol (acetaminophen) |
|
12 AM (MIDNIGHT) |
600 mg Advil (ibuprofen) 1000 mg Tylenol (acetaminophen) |
|
DR. ROTH’S SUGGESTED OVER-THE-COUNTER PAIN REGIMEN SIGNIFICANT PAIN DO NOT take the Tylenol if your opiate has acetaminophen in it already (e.g. Percocet, Norco)
|
|
|
6 AM |
600 mg Advil (ibuprofen) |
|
9 AM |
1000 mg Tylenol (acetaminophen) |
|
12 NOON |
600 mg Advil (ibuprofen) |
|
3 PM |
1000 mg Tylenol (acetaminophen) |
|
6 PM |
600 mg Advil (ibuprofen) |
|
9 PM |
1000 mg Tylenol (acetaminophen) |
|
12 AM (MIDNIGHT) |
600 mg Advil (ibuprofen) |
|
3 AM |
1000 mg Tylenol (acetaminophen) |
Note that this regimen is the same as the “Moderate Pain” regimen, however, it splits the Advil and the Tylenol so that they are taken at different times. In this regimen, you are taking SOMETHING every 3 hours, so you are always on the “upswing” of one or the other medication. Just as one of the medications is wearing off, you are dosing yourself with the other medication.
IN ADDITION to the “Over-The-Counter” pain regimens above, the opiate you have been prescribed (typically oxycodone) can be added in AS NEEDED to supplement your pain and manage breakthrough moments of increased pain. You are encouraged to try to stop taking the opiate as soon as possible, and if you can manage without the opiate, please feel free to do so. At each moment that you are taking your other medications, try to assess your level of pain and take an oxycodone
|
SUGGESTED PAIN REGIMEN – WITH OPIATE MODERATE PAIN |
|
|
6 AM |
600 mg Advil (ibuprofen) 1000 mg Tylenol (acetaminophen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
12 PM (NOON) |
600 mg Advil (ibuprofen) 1000 mg Tylenol (acetaminophen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
6 PM |
600 mg Advil (ibuprofen) 1000 mg Tylenol (acetaminophen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
12 AM (MIDNIGHT) |
600 mg Advil (ibuprofen) 1000 mg Tylenol (acetaminophen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
SUGGESTED PAIN REGIMEN – WITH OPIATE SIGNIFICANT PAIN *** If you are following this regimen, and are consistently taking TWO oxycodone at EACH time point, please call Dr. Roth to let him know that you are requiring that level of pain relief. ***
|
|
|
6 AM |
600 mg Advil (ibuprofen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
9 AM |
1000 mg Tylenol (acetaminophen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
12 NOON |
600 mg Advil (ibuprofen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
3 PM |
1000 mg Tylenol (acetaminophen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
6 PM |
600 mg Advil (ibuprofen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
9 PM |
1000 mg Tylenol (acetaminophen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
12 AM (MIDNIGHT) |
600 mg Advil (ibuprofen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
|
3 AM |
1000 mg Tylenol (acetaminophen) + Pain Level 0-4: NO Oxycodone Pain Level 5-7: ONE Oxycodone Pain Level 8-10: TWO Oxycodone |
Do NOT drive a car or operate any heavy machinery while you are taking narcotic pain medication
(OxyCODONE, Oycontin, Norco, Percocet, Tylenol #3, etc.)
ACTIVITY
- Sleeping is likely to be the most comfortable sitting in a slightly upright position either in a reclining chair (e.g. Lazy-Boy) or on the bed with 4 or 5 pillows stacked up behind your back. You may also want to place a pillow under your forearm to support the arm.
- Avoid any activities which increase pain and swelling such as lifting things, or prolonged periods of standing standing/walking for the first 7-10 days after surgery as these activities are likely to increase the swelling of your arm.
- Avoid long periods of sitting without the arm supported, or long distance travel for 2 weeks after surgery if possible.
- No driving until discussed in the office with Dr. Roth.
- You may return to sedentary work / school 3-4 days after surgery if swelling and pain are tolerable and you are no longer taking narcotic pain medications.
- DO NOT SMOKE cigarettes, smokeless tobacco, cigars, dip, chew, or any other tobacco product for at least 3 months after surgery if at all possible, as these will all inhibit healing of the repair, increase the risk of infection, and decrease the ability of the wound to heal.
SLING (IMMOBILIZER)
- Dr. Roth has a helpful video on his website at www.ROTHSportsMed.com under the “Media” tab where he explains a technique for putting on your shoulder sling by yourself.
- Dr. Roth will let you know at your first post-operative visit exactly what the entire duration of sling use will be for your particular surgery, but it will usually be for 4-6 weeks.
- Until you are seen at your first post-operative visit, the sling is to be worn at all times, but may be removed for the following activities: hygiene (e.g. showering), exercises (described below), eating, using a computer, or reading.
- WEAR SLING WHILE SLEEPING
- Putting the sling on and taking it off can take some practice, and it is usually easiest to do it first a few times with someone helping you. After a while, you will likely get very good at doing it yourself. Many patients find it easiest to leave the shoulder strap clipped together, and place the sling with the pillow attached onto a table or countertop, and then to use the good arm to place the operative arm into the sling, resting it on the table. Then, with the injured arm supported by the table, the good arm can reach over and grab the shoulder strap and pull it over your head. (SEE VIDEO AT WWW.ROTHSPORTSMED.COM)
ICE THERAPY
- Dr. Roth highly recommends purchasing an ice machine for the post-operative period as it is much more convenient than ice packs, however, if necessary, ice packs are sufficient as well.
- Start ice immediately after surgery. You may initially have a bulky dressing on your shoulder and therefore you may not feel like the cold is penetrating, but it is still helping.
- Ice for 20 minutes a minimum of four times daily, or more often if you prefer, but no more often than 20 minutes every hour. Be sure there is always something between the ice pack and your skin and do NOT ice for longer than 20 minutes at a time or you could get frostbite.
- If you had a block at the time of surgery, your shoulder and arm may be numb for up to 24 hours. It is particularly important during this time to be aware of the clock when you are icing as you will not feel the cold and frostbite is a real concern.
EXERCISE

- Unless instructed otherwise by Dr. Roth, you may start your exercises 24 hours after surgery.
- Pendulums
- Bend over at the waist and let the arm dangle. Rock your body in a circular and side to side motion and try to think about letting the arm go completely limp, like a wet noodle. Try to avoid using the muscles of the arm to initiate movement but rather use the rocking motion of your body so that the arm swings, like a pendulum.

- Shoulder Shrugs
- Shrug shoulders upward
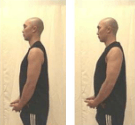
- Shoulder blade pinches
- Pinch shoulder blades together
- Move wrist and fingers
- Bend and straighten elbow (if you had a biceps tenodesis, no ACTIVE elbow flexion until 4 weeks after surgery, but OK to use other hand to bend and straighten the elbow passively)
- Try to do your exercises a minimum of 3 times per day after surgery, more is OK.
- Formal outpatient physical therapy will usually begin at around 2 weeks from surgery, depending on your surgery.
- At one week after surgery, it is OK to begin generalized conditioning, e.g. gentle exercise bike, going for walks, etc.
EMERGENCIES
- Ideally, contact Dr. Roth’s office at 650-853-2943 during business hours to reach Dr. Roth or a representative.
- For concerns that cannot be addressed during business hours, call the Muir Orthopaedic Specialists Call Center at 650-853-2943.
- Please contact Dr. Roth’s office immediately if any of the following are present, or for any other concerns:
- Pain that is not controlled by the regimen described above
- Pain that is unrelenting or getting worse over time rather than staying the same or improving
- Numbness that lasts longer than 24 hours after surgery
- Fever (greater than 101⁰ - low grade fever is normal for the first few days after surgery)
- Redness around the incisions
- Continuous drainage or bleeding from the incision (some drainage is expected)
- Difficulty breathing
- Chest Pain
- Light headedness or passing out
- Uncontrollable nausea, vomiting
- Color change in the operative extremity
- Blistering of the skin
- If you have an emergency that requires immediate attention, proceed to the nearest Emergency Room.
FOLLOW-UP
- If you do not already have a follow-up appointment scheduled, please call 650-853-2943 to schedule an appointment. Follow-up appointments are generally 7-10 days after surgery.









